The Heterogeneous Prostate Gland: Unlocking Its Secrets
What if the key to understanding prostate health lies in its complexity? The prostate gland is a vital part of the male reproductive system. It surrounds the urethra and plays a key role in ejaculation.
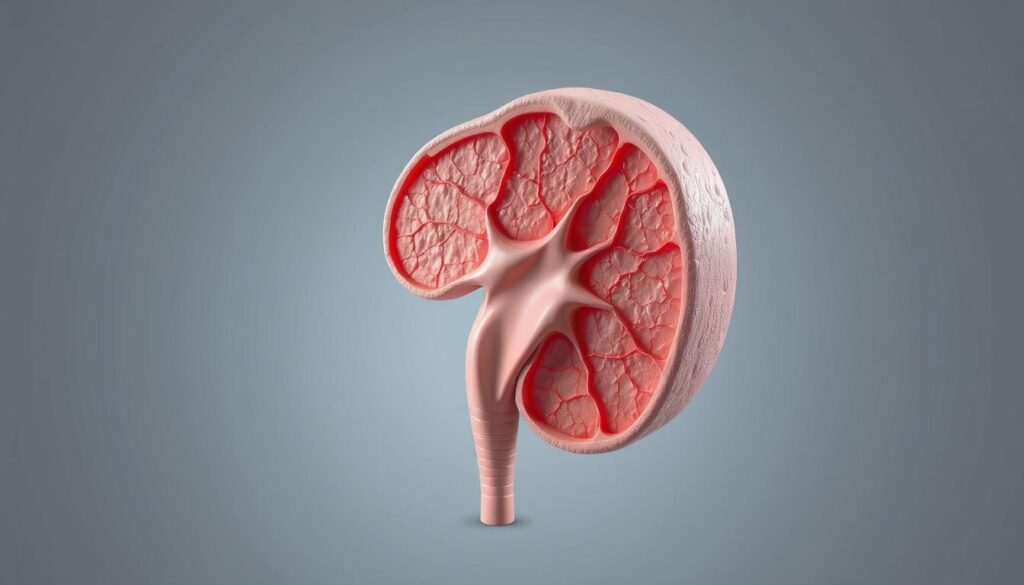
The concept of heterogeneous prostate gland refers to its complex and varied tissue structure. Understanding this complexity is key for diagnosing and treating prostate-related conditions, like Benign Prostatic Hyperplasia (BPH).
As we explore the prostate’s heterogeneity, we’ll look at its different zones and the roles of various cells. We’ll see how these factors impact prostate health and disease.
Key Takeaways
- Understanding prostate heterogeneity is vital for accurate diagnosis and effective treatment.
- The complex structure of the prostate gland makes managing prostate health challenging.
- This article will cover the anatomy, imaging techniques, and treatment approaches for prostate conditions.
- Recognizing prostate heterogeneity is key in both clinical practice and research.
- Knowledge of prostate heterogeneity benefits both patients and healthcare providers.
Understanding the Prostate Gland: Anatomy and Function
The prostate gland is a walnut-sized organ that is integral to the male reproductive system. It has a complex anatomy and multiple functions. As we explore the prostate, it’s clear that its anatomy and physiological roles are closely intertwined.
Basic Anatomy of the Prostate
The prostate gland is located just below the bladder, surrounding the urethra. The urethra is the tube that carries urine from the bladder out of the body. This gland is about the size of a walnut in young men but can enlarge with age.
The prostate is composed of glandular tissue, fibrous tissue, and smooth muscle. The glandular tissue produces prostatic fluid, which is a significant component of seminal fluid.
The Four Zones of the Prostate
The prostate is divided into four zones: the peripheral zone, transition zone, central zone, and anterior fibromuscular zone. The peripheral zone is the largest part and is the most common site for prostate cancer. The transition zone is the area that enlarges in benign prostatic hyperplasia (BPH).
Understanding these zones is critical for diagnosing and treating prostate conditions effectively.
Physiological Functions
The prostate plays a vital role in male fertility by producing some of the fluid that carries sperm during ejaculation. This prostatic fluid constitutes about 30% of the seminal fluid volume and contains enzymes, zinc, and citric acid that support sperm viability and function.
During ejaculation, the prostate’s smooth muscle contracts to help propel seminal fluid into the urethra. The prostate is also involved in hormone metabolism, converting testosterone to dihydrotestosterone (DHT) by the enzyme 5-alpha reductase. This process is significant for the development and maintenance of male sexual characteristics and is a target for certain treatments for prostate conditions.
In this article, we will explore how understanding the prostate’s physiological functions is essential for developing effective treatment strategies for various prostate conditions while minimizing side effects in patients. The heterogeneity of the prostate gland, in terms of its cellular composition and function, adds complexity to its diagnosis and treatment.
What Makes the Prostate Heterogeneous?
Heterogeneity in the prostate gland refers to the variations in its tissue composition and structure. This concept is key in understanding the various conditions that affect the prostate, including benign prostatic hyperplasia (BPH) and prostate cancer.
Definition of Heterogeneity in Prostate Tissue
The term “heterogeneity” in the context of the prostate gland refers to the diverse characteristics of its tissue. This includes variations in cellular composition, glandular structure, and stromal elements. This diversity is a hallmark of the prostate’s complex anatomy and is influenced by hormonal influences and age-related changes.
Prostate tissue heterogeneity can be observed at multiple levels, from the overall zonal anatomy to the specific cellular and molecular characteristics of the gland. Understanding this heterogeneity is essential for accurate diagnosis and effective treatment of prostate conditions.
Cellular Diversity Within the Prostate
The prostate gland has different cell types like epithelial, stromal, and neuroendocrine cells. Each type has its own role and characteristics. For example, epithelial cells make prostatic secretions, while stromal cells give the gland its structure.
This mix of cells makes the prostate diverse and important for its normal work. Changes in these cells can cause problems like BPH and prostate cancer.
Age-Related Changes in Prostate Heterogeneity
Age affects the prostate’s diversity. Around 40, the prostate’s transition zone starts growing slowly. This growth gets faster with age, leading to bigger prostate sizes and changes in its zones.
This can cause BPH in many older men. Understanding these changes helps tell normal aging from serious health issues.
The Cellular Architecture of the Heterogeneous Prostate Gland
Knowing the prostate’s cell makeup is key to understanding its complexity. The prostate gland has various cell types that work together for its function.
Epithelial Cell Types and Hierarchy
The prostate’s epithelial cells include basal, luminal, and neuroendocrine cells. Luminal cells are the most common and make prostatic secretions. Basal cells help keep the epithelial layer intact. The way these cells work together is essential for the prostate’s health.
Stromal Components and Their Roles
The stromal part of the prostate has smooth muscle cells, fibroblasts, and extracellular matrix. It supports the prostate’s structure and helps control epithelial cell behavior. The interaction between stromal and epithelial cells is vital for keeping the tissue balanced.
Stem Cells and Progenitor Populations
Research shows the prostate has stem cells and progenitor populations for regeneration and maintenance. John Isaacs first found these cells in the 1980s through experiments. These cells are androgen-independent and play a big role in prostate cancer development.
| Cell Type | Function | Role in Disease |
|---|---|---|
| Luminal Cells | Produce prostatic secretions | Potential origin of prostate cancer |
| Basal Cells | Maintain epithelial layer | May contribute to cancer development |
| Stem Cells | Regeneration and maintenance | Potential cells of origin for cancer |
Prostate Zones and Their Unique Characteristics
The non-diseased human prostate has four main zones. These zones are the peripheral zone, transition zone, central zone, and anterior fibromuscular stroma. Each zone has its own role in prostate health.
Peripheral Zone: Features and Susceptibility
The peripheral zone is where most prostate cancers start. It’s located at the back and sides of the prostate. Its size and glandular tissue make it more prone to cancer.
Transition Zone: The Site of BPH Development
The transition zone is where Benign Prostatic Hyperplasia (BPH) often starts. It’s around the urethra and can grow with age. This growth can cause urinary problems. Knowing about the transition zone’s role in BPH is key to managing it.
Central and Anterior Fibromuscular Zones
The central zone is around the ejaculatory ducts and makes up about 25% of the prostate. It has a complex ductal system and special cells. The anterior fibromuscular stroma is not glandular, made mostly of smooth muscle and fibrous tissue. These areas have unique features and play important roles in prostate health and disease.
| Prostate Zone | Characteristics | Disease Susceptibility |
|---|---|---|
| Peripheral Zone | Glandular tissue, posterior and lateral location | High risk for prostate cancer |
| Transition Zone | Surrounds the urethra, enlarges with age | Common site for BPH development |
| Central Zone | Surrounds ejaculatory ducts, complex ductal system | Less common for cancer, but potentially aggressive |
| Anterior Fibromuscular Stroma | Non-glandular, smooth muscle, and fibrous tissue | Not typically associated with cancer or BPH |
Imaging the Heterogeneous Prostate Gland
Advanced imaging, like multi-parametric MRI, has changed how we see the prostate gland. It gives a detailed look at the prostate’s anatomy and spots possible problems.
Multi-parametric MRI Techniques
Multi-parametric MRI (mpMRI) uses different MRI sequences for a full prostate check. It includes T2-weighted imaging, diffusion-weighted imaging, and dynamic contrast-enhanced imaging. This way, doctors can see the prostate’s differences and find any suspicious spots.
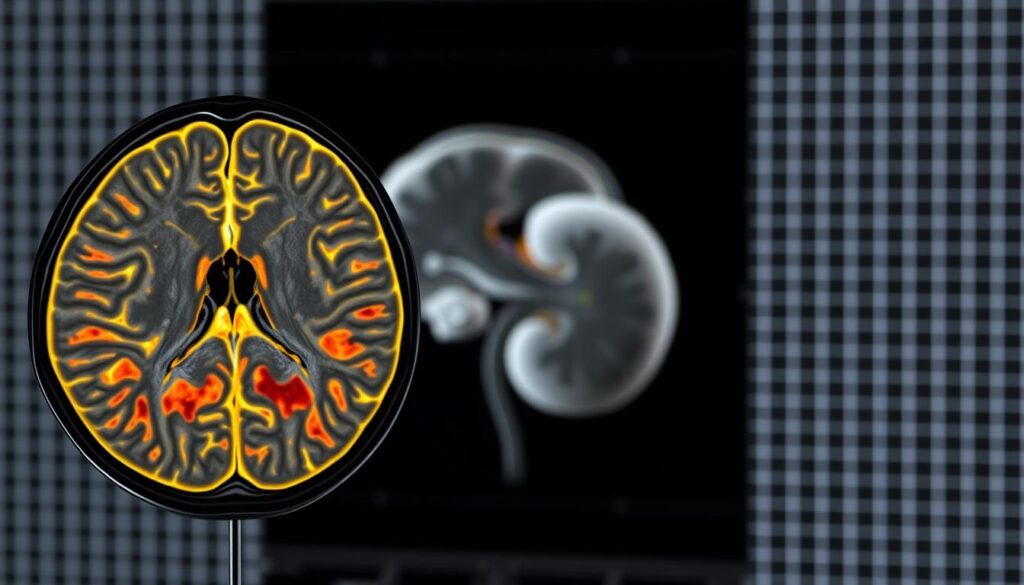
Interpreting Heterogeneity on Imaging
Looking at prostate mpMRI images can be tricky because of the gland’s differences. Normal prostate variations can look like disease, leading to wrong diagnoses. For example, BPH nodules in the transition zone might look like cancer.
Challenges in Image Interpretation
Prostate heterogeneity on mpMRI can cause both wrong and missed diagnoses. Conditions like prostatitis or post-biopsy bleeding can make images hard to read. Things like the MRI’s strength and the coil used also affect image quality. Systems like PI-RADS help by making image reading more consistent.
| Challenge | Description | Impact on Interpretation |
|---|---|---|
| Normal heterogeneity mimicking pathology | BPH nodules resembling cancer | False-positive interpretations |
| Post-biopsy changes | Hemorrhage or inflammation | Complicated signal patterns |
| Technical factors | Magnetic field strength, coil selection | Affects image quality |
Benign Prostatic Hyperplasia (BPH): A Manifestation of Heterogeneity
Benign Prostatic Hyperplasia (BPH) shows how different the prostate gland can be. As men get older, the prostate changes a lot, leading to BPH in many cases. This condition makes the prostate bigger, causing urinary problems.
Pathophysiology of BPH
BPH happens when the prostate gland grows, mainly in the transition zone. This growth starts around 40 years old and speeds up with age. It’s caused by cells multiplying and changes in the prostate’s structure.
Treatment with 5-alpha reductase inhibitors (5ARIs) can shrink the prostate. On average, it reduces by 19% in patients, slowing down symptoms.
Different Phenotypes of BPH
BPH isn’t the same for everyone. It mainly grows in the transition zone. In young men, this zone is small, but in older men, it can grow a lot.
Impact on Prostate Volume and Structure
BPH changes the prostate’s size and shape. It can grow from 20g to over 60g. This can block the urethra and make it hard to find cancer.
| Characteristics | Normal Prostate | Prostate with BPH |
|---|---|---|
| Prostate Volume | Approximately 20g | 60g or more |
| Transition Zone | 5% of prostate volume | More than 50% of prostate volume |
| Impact on Urethra | Minimal distortion | Significant distortion |
Prostate Cancer and Tissue Heterogeneity
Understanding prostate cancer is key to better treatments. It’s complex, with different cells and genes. This makes it hard to treat.
Also Check prostate gland histology
How Heterogeneity Affects Cancer Development
Prostate cancer varies a lot. Different parts of the prostate can grow into cancer in different ways. For example, cancers in the central zone might act differently than those in the peripheral zone.
Intratumoral heterogeneity means tumors can behave differently. This makes treatment tricky.
Challenges in Cancer Detection Due to Heterogeneity
Finding prostate cancer is hard because of its variety. Tumors can look and act differently. New tests, like genomic testing, are being used to understand this better.
Prognostic Implications
How prostate cancer behaves can depend on its type. Some cancers are more aggressive than others. Knowing this helps doctors plan better treatments.
Understanding prostate cancer is essential for better care. New tests and treatments are being developed to tackle its complexity.
Prostatitis and Inflammation in the Heterogeneous Gland
Prostatitis is an inflammation of the prostate gland. It affects men differently. This condition can cause various symptoms and problems, affecting men’s health and life quality.
Types of Prostatitis
Prostatitis is divided into types based on its causes and symptoms. The main types are acute bacterial prostatitis, chronic bacterial prostatitis, chronic prostatitis/chronic pelvic pain syndrome, and asymptomatic inflammatory prostatitis. Each type needs a different approach to diagnosis and treatment.
For example, acute bacterial prostatitis is caused by a bacterial infection and has severe symptoms. On the other hand, chronic prostatitis/chronic pelvic pain syndrome is characterized by ongoing pain and discomfort without clear bacterial infection signs.
Relationship Between Inflammation and Heterogeneity
Inflammation in the prostate gland can change its cellular makeup and structure. This leads to increased heterogeneity. The presence of immune cells and changes in tissue populations contribute to this.
Dr. John Smith, a urologist, notes, “Chronic inflammation can cause tissue remodeling and hyperplastic growth. This creates a microenvironment that may lead to BPH and prostate cancer.”
Inflammation can cause focal areas of atrophy, hyperplasia, and metaplasia in the glandular and stromal compartments. This increases prostate heterogeneity. On imaging studies, like MRI, inflammation can create signal abnormalities that mimic other conditions, making diagnosis hard.
Diagnostic Approaches for the Heterogeneous Prostate
The heterogeneous prostate gland is challenging to diagnose. A multifaceted approach is needed. Accurate diagnosis is key for effective patient care and treatment planning.
Digital Rectal Examination (DRE)
A Digital Rectal Examination (DRE) is a basic diagnostic tool for the prostate gland. During a DRE, a healthcare provider feels the prostate to find abnormalities. While not definitive alone, a DRE provides valuable information when combined with other tests. It’s useful for detecting abnormalities in the prostate’s posterior aspect.
PSA Testing and Its Limitations
Prostate-Specific Antigen (PSA) testing is a blood test for prostate cancer screening. Elevated PSA levels can indicate prostate issues, including cancer, prostatitis, or BPH. But, PSA testing has limitations, like false positives and lack of specificity for cancer.
Not all men with elevated PSA have cancer, and some with prostate cancer may have normal PSA levels. So, PSA testing is often used with other diagnostic approaches to improve accuracy.
Advanced Biomarkers for Heterogeneous Tissue
Advanced biomarkers are promising for diagnosing prostate conditions. These include blood, urine, and tissue biomarkers that can better characterize the heterogeneous prostate tissue. For example, the Prostate Health Index (phi) and 4Kscore are biomarker panels that improve diagnostic performance beyond PSA alone.
Tissue-based biomarkers, like immunohistochemical markers and gene expression profiles, can help in characterizing prostate cancer heterogeneity and predicting disease behavior. Liquid biopsy approaches, including circulating tumor cells and cell-free DNA analysis, offer non-invasive assessment of prostate cancer heterogeneity.
By integrating biomarker data with clinical and imaging information, healthcare providers can achieve a more complete assessment of the heterogeneous prostate. This guides clinical decision-making and may improve patient outcomes.
Biopsy Strategies for the Heterogeneous Prostate
Effective biopsy strategies are essential for the heterogeneous prostate gland. The prostate’s variability in tissue composition and different zones make accurate diagnosis of conditions like prostate cancer challenging.
Systematic Biopsy vs. MRI-Directed Target Biopsy
The debate between systematic biopsy and MRI-directed target biopsy is ongoing. Each method has its own benefits. Systematic biopsy takes many samples from different parts of the prostate. This gives a detailed view of the gland’s health.
On the other hand, MRI-directed target biopsy focuses on specific areas of concern. It uses imaging to pinpoint these areas. This could lead to more accurate diagnoses.
Studies have found that TZ ADC heterogeneity affects the choice between systematic biopsy and MRI-directed target biopsy. The transition zone’s ADC heterogeneity was linked to systematic biopsy before adjusting for multiple comparisons (p = 0.032). After adjusting, the p-value was 0.24. This shows that ADC heterogeneity in the transition zone might influence the biopsy method choice.
Combined Biopsy Approaches
To better find cancer, doctors use a mix of biopsy methods. They combine systematic and MRI-directed biopsies. This mix aims to improve how well they can spot cancer.
There are different ways to do this, depending on how many samples are taken and where. Also, how they target MRI-visible spots can vary.
- Studies show that this mix can find more important prostate cancer than either method alone.
- This mix is good because the prostate is not the same everywhere. Some cancers might not show up on MRI.
- People with past negative biopsies, high PSA levels, or uneven prostate on MRI might get the most benefit.
But, there are downsides. It might cost more and could lead to finding cancers that aren’t a big deal. It might also cause more problems because of more samples taken.
Clinical Implications of Prostate Heterogeneity
The prostate gland is not the same everywhere. This fact changes how we treat prostate problems. As we learn more about this, we’ll find better ways to diagnose and treat.
Impact on Symptom Presentation
Because the prostate is different, symptoms can vary. For example, how big and where the prostate is can affect urinary problems. MRI can help see these differences, which might help understand symptoms better.
Challenges in Clinical Management
Dealing with prostate issues is hard because of its differences. Different problems need different treatments. The 2008 NIDDK Prostate Strategic Plan said we need treatments that match the problem.
Personalized Approaches Based on Heterogeneity
Now, doctors are trying to treat each person differently. They use things like age and health problems, along with what the prostate looks like. For example, tests can help decide how strong to treat prostate cancer. This shows how personalized medicine can work.
| Prostate Condition | Impact of Heterogeneity | Personalized Approach |
|---|---|---|
| BPH | Varied symptom presentation | Medication selection based on prostate size and symptom type |
| Prostate Cancer | Differential treatment response | Genomic testing to guide treatment intensity |
| Prostatitis | Variable inflammatory responses | Targeted anti-inflammatory therapies |
Medical Management of Heterogeneous Prostate Conditions
Handling different prostate issues needs a mix of treatments. Because of the prostate’s complexity, a detailed plan is needed. This plan considers what’s specific to the patient’s prostate.
Alpha-1 Blockers: Mechanism and Efficacy
Alpha-1 blockers are a main treatment for urinary problems linked to BPH. They relax muscles in the prostate and bladder neck. This makes it easier to pee and reduces symptoms.
5-Alpha Reductase Inhibitors (5ARIs)
5ARIs are key for BPH treatment. They stop testosterone from turning into DHT, a hormone that makes the prostate grow. This reduces prostate size and helps symptoms.
Combination Therapy Approaches
Using alpha-1 blockers and 5ARIs together helps more than using one alone, mainly for men with big prostates. Studies like MTOPS, CombAT, and PREDICT show this combo stops the disease from getting worse.
| Therapy Approach | Mechanism | Efficacy |
|---|---|---|
| Alpha-1 Blockers | Relax smooth muscles | Rapid symptom relief |
| 5ARIs | Inhibit DHT production | Reduce prostate volume |
| Combination Therapy | Targets both dynamic and static obstruction | Superior symptom relief and disease progression prevention |
Patient selection is critical for combination therapy. It works best for men with big prostates, high PSA levels, and bad symptoms.
New combos are being tried, like alpha-1 blockers with other drugs. They aim to tackle different parts of urinary problems.
Surgical Interventions for Prostate Conditions
Surgery is key for prostate issues, helping those with urinary blockages and other problems. The right surgery depends on the prostate size, the patient’s health, and the problem being treated.
Transurethral Resection of the Prostate (TURP)
TURP is a common surgery for BPH. It removes parts of the prostate blocking urine. Done under anesthesia, it’s a big step but offers lasting relief. Yet, it can lead to bleeding, infection, and affect sex life.
Simple Prostatectomy
Simple prostatectomy is for big prostates or when other treatments fail. It removes the prostate’s inner part. It’s effective but riskier than less invasive methods.
Minimally Invasive Surgical Options
New, less invasive surgeries are available. These include laser treatments, thermal therapies, and new methods like UroLift and Rezūm. They aim to reduce risks while solving the problem.
| Procedure | Description | Benefits |
|---|---|---|
| TURP | Removes obstructing prostate tissue | Significant symptom relief |
| HoLEP | Laser enucleation of the prostate | Effective for large prostates, less bleeding |
| UroLift | Lifts the prostate tissue away from the urethra | Minimally invasive, preserves sexual function |
Future Directions in Understanding Prostate Heterogeneity
Prostate research is getting a boost from new tech. We’re learning more about the prostate and finding new ways to diagnose and treat. This section looks at the future, including single-cell sequencing, AI in imaging, and treatments based on cell types.
Single-Cell Sequencing Technologies
Single-cell sequencing is changing how we see prostate cells. It lets researchers find out which cells are important in health and disease. This helps create treatments that target specific cells, not just the whole prostate.
Studies have found certain cells are more common in prostate cancer. This gives doctors new targets for treatments.
Artificial Intelligence in Imaging Analysis
Artificial intelligence (AI) is making medical imaging better. AI finds patterns in images that show prostate problems like cancer. This makes early detection and treatment more accurate.
AI also helps tailor treatments to each patient. It looks at patient data to predict how well they’ll respond to treatments.
Targeted Therapies Based on Cellular Phenotypes
Researchers are working on treatments that target specific prostate cells. This approach could make treatments more effective and reduce side effects. For example, they’re looking at therapies for BPH and cancer cells.
Using biomarkers, doctors can choose the best treatment for each patient. This could lead to more personalized care.
The Role of Heterogeneity in Treatment Response
The prostate gland’s diversity affects how treatments work. Different tissues and cells in the prostate can react differently to treatments.
Studies show that treatments don’t work the same for everyone. Some patients see big improvements, while others don’t. This shows how important it is to understand the prostate’s diversity when planning treatments.
Predictors of Treatment Success
Finding out who will respond well to treatments is key. A patient’s health, prostate tissue, and other health issues can affect how well they do. Knowing these factors helps doctors choose the best treatment for each patient.
Some biomarkers and genetic markers can also predict treatment success. For example, certain genetic changes can make some treatments work better. By finding these markers, doctors can make better treatment choices.
Overcoming Treatment Resistance
Prostate diversity can also lead to treatment resistance. Different cells in the prostate may react differently to treatments, leading to resistant cells.
To fight resistance, doctors might try different treatments or add new medications. For surgeries, dealing with leftover tissue can help keep symptoms away. Personalized treatments can improve results.
A leading researcher once said,
“The key to overcoming treatment resistance lies in understanding the complex interplay between prostate heterogeneity and therapeutic interventions.”
This knowledge is key to better treatments for prostate conditions.
By understanding how diversity affects treatment, we can improve care for prostate patients. This leads to better outcomes and better care for those with prostate issues.
Conclusion
The heterogeneous prostate gland needs a complex approach for health management. This includes diagnosis and treatment. In this article, we’ve looked into the prostate’s anatomy and how it changes. We’ve seen how its differences make treatment hard.
Knowing about prostate heterogeneity helps us create better treatments for different prostate issues. This shift from a one-size-fits-all approach to personalized care is key. It’s changed how we diagnose and treat patients.
The impact of heterogeneity is big for both patients and doctors. It helps in better patient care and treatment choices. But, we need better biomarkers and imaging, and more targeted treatments.
Research and clinical care are moving forward to tackle heterogeneity. This could lead to better, more tailored care for prostate issues. We urge more research and innovation in this area. It could greatly help the millions of men with prostate problems worldwide.
By learning more about the heterogeneous prostate gland, we can improve care for patients. This will make prostate health management better for everyone.
FAQ
What is prostate heterogeneity, and why is it significant?
Prostate heterogeneity means the prostate has different cells and tissues. This diversity is important because it affects prostate diseases like cancer and BPH.
How does age affect prostate heterogeneity?
As men get older, the prostate changes. This leads to more heterogeneity, including BPH and changes in cell types.
What role does the peripheral zone play in prostate health?
The peripheral zone is where most prostate cancers start. It’s very important for checking and diagnosing prostate health.
How do different imaging techniques help in understanding prostate heterogeneity?
Techniques like multi-parametric MRI help see and study prostate heterogeneity. They help find and manage prostate diseases.
What is the significance of PSA testing in the context of prostate heterogeneity?
PSA testing is good for finding prostate cancer. But, it has limits, so we need more tests to understand heterogeneity.
How do biopsy strategies address the challenges posed by prostate heterogeneity?
Biopsy methods, like systematic and MRI-directed biopsies, help diagnose prostate diseases. They work well with heterogeneity.
What are the implications of prostate heterogeneity for treatment?
Heterogeneity can affect how treatments work. This means we need treatments that fit each person’s needs.
How do alpha-1 blockers and 5-alpha reductase inhibitors work in managing BPH?
Alpha-1 blockers relax muscles to improve urine flow. 5-alpha reductase inhibitors shrink the prostate by blocking DHT. Both help with BPH symptoms.
What are the future directions in understanding and managing prostate heterogeneity?
New technologies like single-cell sequencing and AI in imaging will change how we understand and manage prostate heterogeneity.


Post Comment