Prostate Gland Histology: A Detailed Observation
Have you ever wondered what makes the prostate gland so important for male health?
The prostate is a complex organ. It has glandular and fibromuscular tissue. It plays a key role in making seminal fluid. Knowing its histological structure is vital for diagnosing and treating prostate issues.
Understanding the normal prostate helps avoid mistaking it for cancer. The prostate’s microscopic anatomy will be examined. This includes its cellular organization and zonal architecture.
Key Takeaways
- The prostate gland is vital for male reproductive health.
- Knowing prostate histology is key to diagnosing and treating prostate conditions.
- The prostate’s unique histological features contribute to its physiological functions.
- Changes in prostate structures can lead to disease.
- Prostate gland histology has significant clinical implications.
Understanding the Prostate Gland
The prostate gland is a key part of the male reproductive system. It plays a vital role in making seminal fluid. We will explore its location, basic structure, and developmental origins to understand this complex organ better.
Location and Basic Structure
The prostate gland is located below the bladder in males. It surrounds the urethra. It has glandular tissue and fibromuscular stroma. The glandular tissue has many ducts that open into the prostatic urethra, playing a key role in secreting prostatic fluid.
The prostate is surrounded by a fibrous capsule. This capsule separates it from surrounding structures. Knowing the prostate’s basic structure is essential for understanding its function and importance in male reproductive health.
Developmental Origins
The development of the prostate gland starts in embryonic development. It arises from the endodermal lining of the urogenital sinus under dihydrotestosterone’s influence. The glandular epithelium of the prostate comes from endodermal cells, while the fibromuscular stroma comes from the surrounding mesenchyme.
Key aspects of prostate development include:
- The prostate gland starts developing in the third month of embryonic life.
- Androgen-dependent development explains why the prostate remains rudimentary in individuals with conditions affecting androgen production or reception.
- The urogenital sinus epithelium forms outgrowths that eventually develop into the prostatic ducts and acini.
| Developmental Stage | Description |
|---|---|
| Embryonic Development | The prostate gland begins to develop from the urogenital sinus. |
| Puberty | Rising testosterone levels trigger significant growth and functional maturation of the prostate. |
| Adulthood | The prostate continues to play a vital role in the male reproductive system. |
Understanding the prostate’s developmental origins helps explain its hormone sensitivity throughout life. It provides insight into the mechanisms of prostate cancer development and progression.
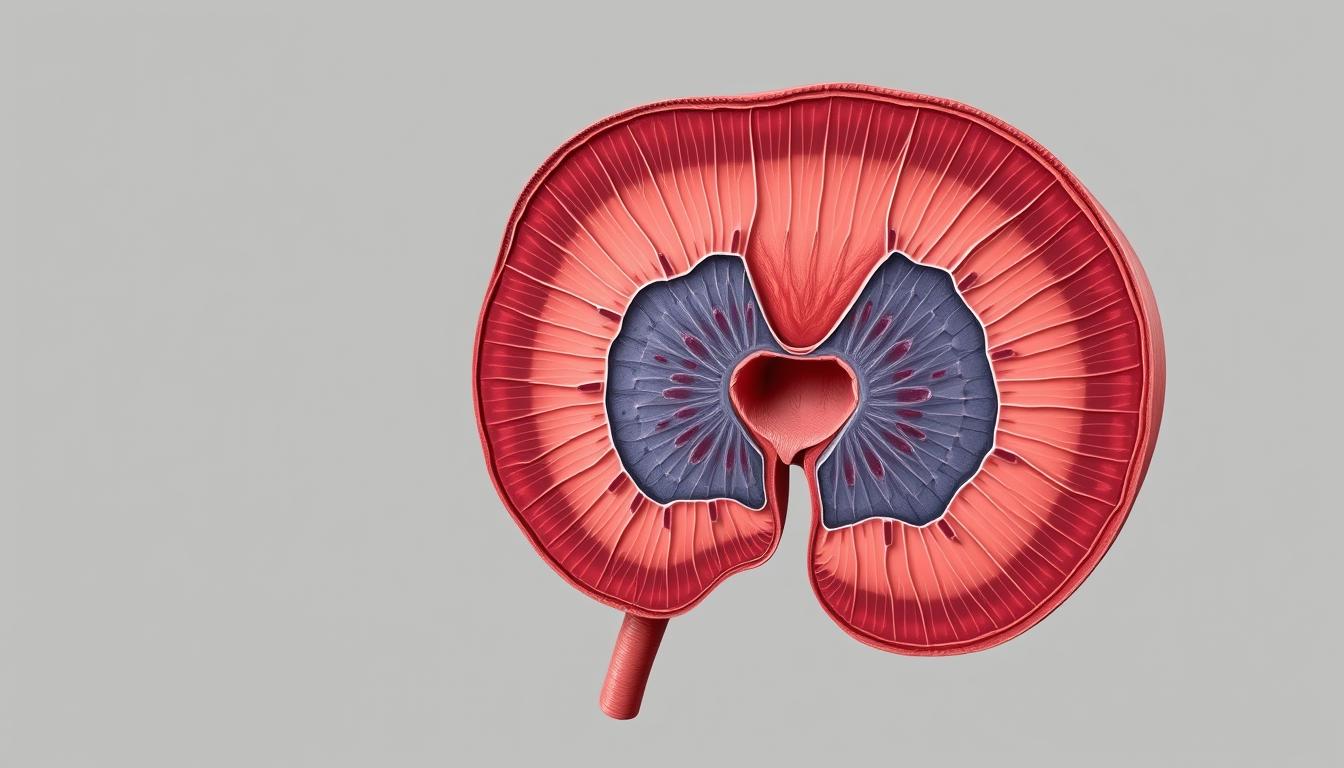
Anatomical Zones of the Prostate
Understanding the prostate’s anatomical zones is key for diagnosing and treating prostate-related diseases. The prostate gland is divided into several zones, each with distinct characteristics and functions.
Peripheral Zone
The peripheral zone is the largest part of the prostate gland, making up about 70% of the glandular tissue. It is located posteriorly and surrounds the distal urethra. This zone is the most common site for prostate cancer, with most tumors starting here. The peripheral zone’s histological structure is characterized by simple, round glands with a prominent lumen.
Central Zone
The central zone accounts for about 25% of the prostate’s glandular tissue and surrounds the ejaculatory ducts. It is cone-shaped, with its base at the prostate’s base and its apex at the verumontanum. The central zone’s glands are more complex, with a larger lumen and more irregular shapes compared to the peripheral zone. This zone is less frequently involved in prostate cancer.
Transition Zone
The transition zone is key in benign prostatic hyperplasia (BPH). It’s around the proximal urethra and makes up about 5% of the gland in young men. But, it can grow a lot with age, sometimes making up to 95% of the gland in older men with BPH.
This zone has mucosal glands and smooth muscle. BPH here can press on the urethra, causing urinary problems.
About 10-20% of prostate cancers start in the transition zone. These cancers often have lower Gleason scores and a better outlook than cancers in other zones.
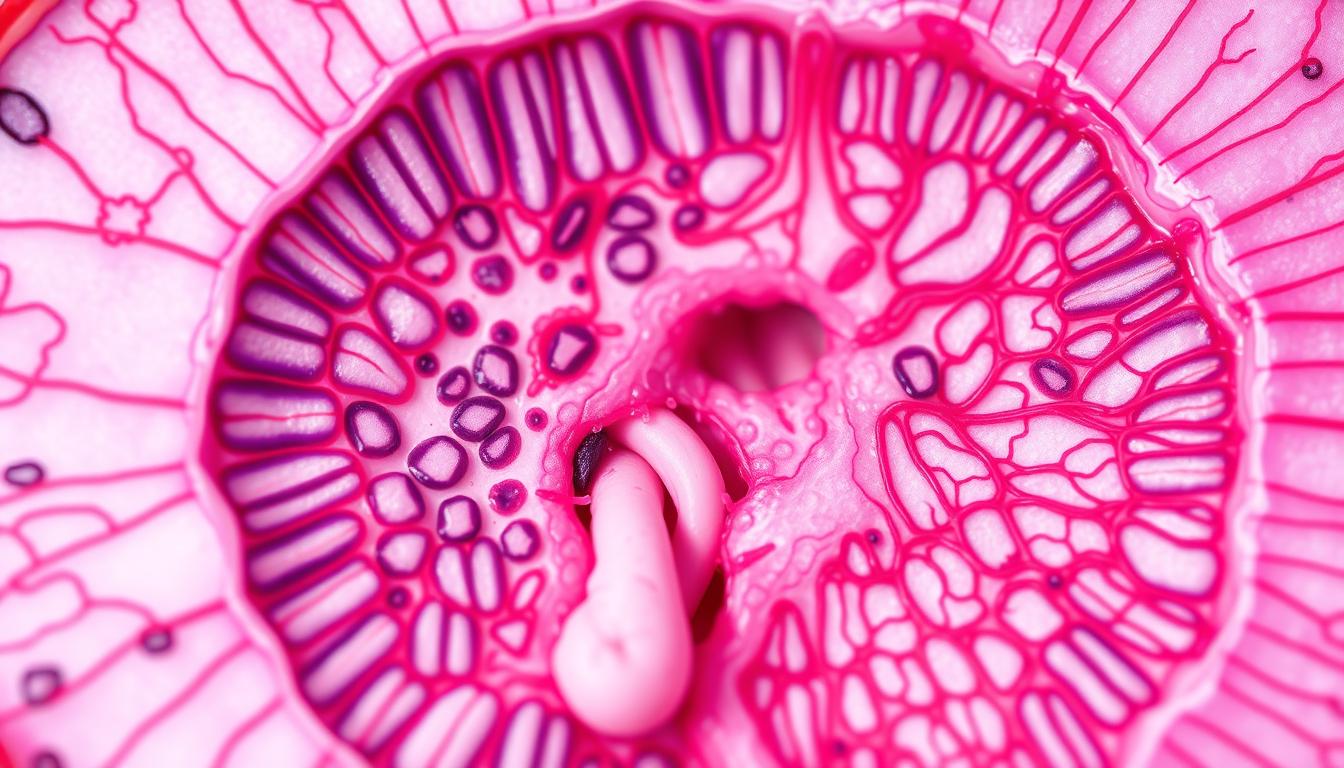
Prostate Gland Histology
The prostate gland’s structure is unique. It has glandular tissue and stromal elements. Knowing about its histology helps us understand its function and diseases.
Glandular Tissue Organization
The prostate gland mainly has glandular tissue. This tissue is organized into tubuloalveolar glands. It’s made of secretory epithelial cells that make prostatic fluid, a key part of semen.
The glandular tissue is in a complex pattern. It has many acini and ducts that lead to the prostatic urethra.
- The glandular tissue is surrounded by a fibromuscular stroma. This stroma supports the gland and helps it contract and release secretions.
- The glandular tissue’s organization changes across different zones of the prostate. The peripheral zone is where most prostate cancers start.
Fibromuscular Stroma
The fibromuscular stroma is a key part of the prostate gland. It has smooth muscle cells and fibroblasts in a collagen and elastic fiber matrix. This stroma helps the gland contract and expel its secretions during ejaculation.
Prostatic Capsules
The prostate gland is covered by two capsular structures. There’s a true internal connective tissue capsule and a false external capsule from the pelvic fascia. The true capsule is a thin layer of collagen, elastic fibers, and smooth muscle cells.
- The true prostatic capsule is thickest posterolaterally and thinnest anteriorly and at the apex. This affects cancer spread.
- The false capsule, or periprostatic fascia, contains the prostatic venous plexus. It surrounds the true capsule, which is important clinically.
Understanding the prostate gland’s histology is key. It helps us grasp its normal function and the changes in diseases.
Cellular Components of the Prostate
Knowing the prostate’s cellular makeup is vital. The prostate gland has various cell types, each with a unique role in its health and function.
Secretory Epithelial Cells
Secretory epithelial cells are key in the prostate gland. They produce prostatic fluid and secrete prostate-specific antigen (PSA) and other proteins. They are essential for the gland’s secretory function.
Basal Cells
Basal cells are under the secretory epithelial cells. They help regenerate the epithelial layer. They are less differentiated than secretory cells and play a role in prostate cancer development.
Neuroendocrine Cells
Neuroendocrine cells are rare in the prostate, making up less than 1% of the cells. They are found throughout the glands and need special stains to see. These cells make hormones like serotonin and bombesin, which help control growth and secretions.
They play a big role in prostate cancer, making it grow faster and harder to treat. This shows how important these cells are in prostate diseases.
Physiological Function and Secretions
The prostate gland is key in the male reproductive system. It makes secretions that help sperm survive and move.
Composition of Prostatic Fluid
Prostatic fluid is made of enzymes, hormones, and proteins. It’s secreted by the glandular cells of the prostate. It’s rich in prostatic specific antigen (PSA), which helps semen liquefy after ejaculation.
The seminal vesicles also add to the seminal fluid. They are surrounded by smooth muscle layers.
Prostatic Concretions
Prostatic concretions, or corpora amylacea, are found in the prostate glands. They grow with age and are made of calcified secretions and cells. They look like round, intensely colored structures with layers.
They are usually harmless but can cause problems if they get too big. They can also cause infections or inflammation.
Forensic pathologists use them to guess a person’s age. They are rare before 40 but common after 50.
Conclusion: Clinical Significance of Prostate Histology
Prostate histology is key in diagnosing and treating prostate issues. It helps doctors understand the zonal anatomy of the prostate. This is important because different zones have different problems.
Histological evaluation is the best way to diagnose prostate cancer. It looks for signs like missing basal cells and unusual cell shapes. The prostate-specific antigen (PSA) is also important, but it’s better with histology.
Knowing about prostate histology has led to better treatments. It helps doctors avoid harming important parts like the seminal vesicles and ejaculatory ducts.
In summary, understanding prostate histology is vital for treating prostate diseases.
FAQ
What is the role of the seminal vesicles in the male reproductive system?
The seminal vesicles are important in the male reproductive system. They make a lot of the fluid in semen, which helps sperm during ejaculation.
What is benign prostatic hyperplasia (BPH), and how does it affect the prostate?
Benign prostatic hyperplasia (BPH) is a non-cancerous growth in the prostate’s transition zone. It can press on the urethra, leading to urinary problems. This condition is common in older men.
What is the significance of the peripheral zone in prostate anatomy?
The peripheral zone is where most prostate cancers start. It’s located at the back and wraps around the central zone.
How does the fibromuscular stroma contribute to prostate function?
The fibromuscular stroma gives the prostate its shape and helps it contract and relax during ejaculation.
What is the relationship between prostate cancer and PSA levels?
High levels of prostate-specific antigen (PSA) in the blood might mean prostate cancer. But, high PSA can also be from BPH or prostatitis.
How does the anatomy of the prostate relate to the urethra and bladder?
The prostate surrounds the prostatic urethra, which links the bladder to the urethral orifice. When the prostate grows, it can squeeze the urethra and change how urine flows.
What is the function of the secretory epithelial cells in the prostate?
The secretory epithelial cells make prostatic fluid. This fluid is a key part of semen and gives sperm the nutrients they need.


Post Comment