Prostatic Artery Embolization: Effective Relief for Enlarged Prostate
Have you wondered if a less invasive option could ease bothersome urinary changes without major surgery?
We offer a modern, minimally invasive treatment for men with enlarged prostate. This procedure uses mean-time imaging and a tiny catheter. It targets blood flow to shrink the prostate over time.
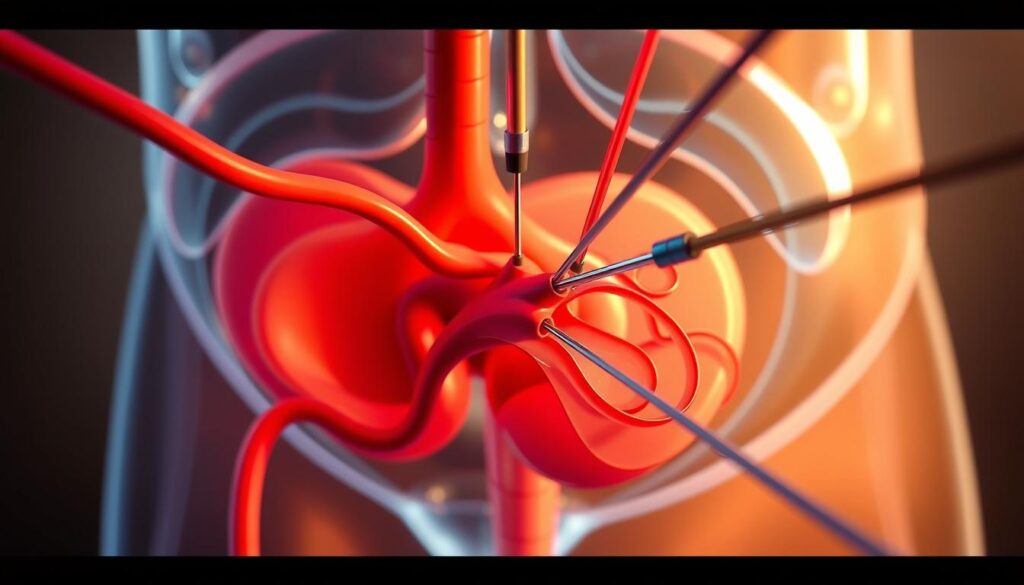
Most patients leave the clinic the same day, with local anesthesia and light sedation. They often see symptom improvement within weeks. Recovery gets better over months.
Our team of subspecialty radiologists guides the evaluation, performs the procedure, and follows patients. We present this option as a proven alternative to surgery. It offers fewer side effects and faster recovery time for men seeking relief.
Key Takeaways
- Prostatic artery embolization is a minimally invasive procedure to reduce prostate enlargement.
- It is imaging-guided and performed by trained interventional radiologists.
- Most patients go home the same day with quick recovery and early symptom relief.
- Outcomes often improve over weeks and can last for years with high satisfaction.
- This treatment offers a surgical alternative for men with urinary tract symptoms from BPH.
What Is Prostatic Artery Embolization and How It Helps BPH
We use tiny catheters and advanced imaging to reduce prostate size without major surgery.
Prostatic artery embolization (PAE) is the treatment. It is a minimally invasive procedure. It reduces blood flow to the prostate gland, causing it to shrink over time. An interventional radiologist performs the procedure using X-ray and 3D imaging to guide a small catheter from the wrist or groin into the target vessels.
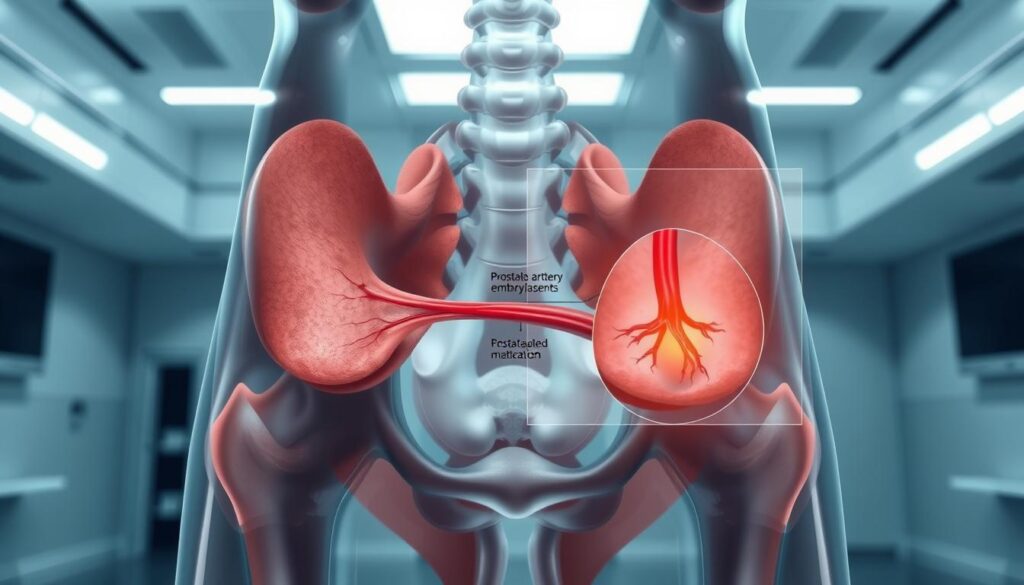
How we do it
- We map vessel anatomy with an arteriogram so we can target both sides precisely.
- Through a microcatheter, tiny microspheres are delivered to block select artery branches.
- Blocking blood flow causes gradual tissue shrinkage and improved urinary flow.
Why patients choose this option
PAE is a nonsurgical, minimally invasive treatment often done with local anesthesia and light sedation. Many men choose this to avoid or delay surgery and to lower the chance of urinary or sexual side effects seen with some operations.
Timing: Symptom relief often begins within weeks as blood supply falls and the prostate remodels. National groups recognize this procedure as an effective option for men with bothersome benign prostatic hyperplasia.
Understanding Benign Prostatic Hyperplasia and Lower Urinary Tract Symptoms
As men age, the prostate often grows and can slowly change how the lower urinary tract works. This noncancerous enlargement — benign prostatic hyperplasia — can press on the urethra and disrupt normal bladder emptying.
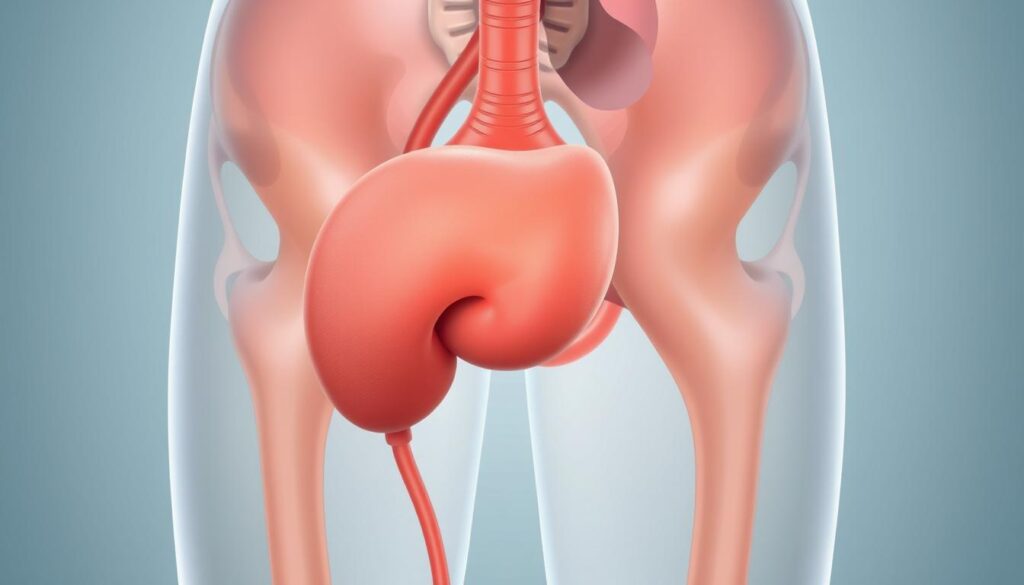
Common signs include increased frequency, sudden urgency, a weak stream, straining to start, and waking to urinate at night (nocturia). These urinary tract symptoms range from mild annoyances to problems that limit activities or sleep.
Chronic outlet obstruction forces the bladder muscle to work harder. Over time, this can cause irritative symptoms and, in some cases, bladder dysfunction or incontinence if untreated.
When symptoms affect daily life
We consider symptoms “bothersome” when they disturb sleep, force constant planning around bathrooms, or cause accidents that reduce confidence. About one in four men have BPH-related complaints by age 55, and roughly half of 75-year-old men report notable issues.
“Timely evaluation can prevent progression and help restore comfort and control.”
- We describe BPH as a benign enlargement that narrows the urethra and disrupts urination.
- We note hallmark lower urinary tract symptoms and how they impact quality of life.
- We explain why reducing prostate bulk often improves flow and lowers bladder strain.
Why Choose a Minimally Invasive Approach Over Surgery
Choosing a less invasive option can make recovery faster and keep your daily life on track. We offer a method that avoids big cuts and often means no hospital stay.
Reduced risk of sexual side effects and urinary incontinence. Prostatic artery embolization has a lower risk of incontinence and fewer sexual side effects. This is good for men who want relief without new problems.
Outpatient care, local anesthesia, and faster recovery. This treatment is often done as an outpatient with local anesthesia. Patients usually feel less pain and can get back to normal faster than surgery.
- No large incision, fewer hospital resources, and a quicker return to routine.
- Evidence shows lower rates of incontinence and sexual side effects versus some surgeries.
- Local anesthesia with light sedation instead of general anesthesia for most patients.
- Outpatient care reduces time away from work and family and lowers overall recovery burden.
- We preserve future options—additional treatments remain possible if needed.
- Board‑certified interventional radiologists perform the procedure using advanced imaging to enhance precision and safety.
We recognize risks exist. Every approach has possible complications. We assist patients in comprehending the advantages and disadvantages of their options so that they can select one that is appropriate for both their health and goals..
Also check prostate gland removal
Am I a Candidate for Prostatic Artery Embolization?
To see if this treatment is right for you, we look at your symptoms and medical history. We check how your urinary issues affect your sleep, work, and life quality.
- Men with moderate to severe urinary symptoms that limit daily activities or cause nocturia.
- Patients who prefer to avoid surgery or who have medical reasons that make general anesthesia risky.
- Those who tried medications or other therapies with limited benefit or intolerable side effects.
- Individuals whose prostate size and anatomy — reviewed on imaging — suggest the procedure may help.
How we decide: An interventional radiologist reviews symptom scores, prior treatments, and imaging. We may use questionnaires to measure symptom burden and set realistic expectations for timing and benefit.
Important: We discuss possible risks and recovery so each recommendation matches personal goals and health.
Pre‑Procedure Evaluation and Imaging Workup
A thorough pre‑procedure workup gives us the roadmap needed for a safe, effective treatment.
We start by documenting symptoms and goals. We use validated symptom scores to measure frequency, severity, and impact on daily life. This helps set realistic expectations for benign prostatic hyperplasia care.
Next, we perform targeted tests to clarify the cause of urine complaints. Typical testing includes urinalysis, a digital rectal exam to assess the prostate gland, and a PSA test when appropriate to rule out other concerns.
Imaging and planning
We obtain ultrasound or MRI to define size, shape, and surrounding anatomy. These scans create an imaging roadmap that guides safe catheter placement during the procedure.
Safety and logistics
- We review medications, including blood thinners, and coordinate temporary adjustments.
- We advise on fasting, arrival time, and arranging a ride home after the clinic visit.
- We counsel on infection prevention and prescribe antibiotics when indicated to lower infection risk.
“A clear clinical picture and precise imaging let our radiologist plan the safest course.”
Prostatic Artery Embolization Procedure: Step‑by‑Step
Here is a clear, practical guide to how we perform the catheter‑based steps used to reduce blood flow to the gland.
We start by numbing the wrist or groin and inserting a small catheter into an artery under live X‑ray guidance.
Our radiologist guides the catheter to the vessels that feed the prostate, using imaging to steer safely and efficiently.
Mapping and targeted delivery
An arteriogram maps the blood flow to find the right spot for treatment.
We inject tiny particles through a tiny catheter to stop blood from getting to the enlarged prostate.
Bilateral treatment and immediate care
We treat both sides at once to tackle the whole gland. The whole process takes about two hours. You’ll be under local anesthesia with some sedation.
After the procedure, we check the site and watch how you’re doing. Most people go home the same day. You might feel some pelvic pain or irritation in your urine, but it should get better in a few days.
“We aim for precise placement and non‑target protection to keep surrounding organs safe.”
Safety Profile, Risks, and Possible Side Effects
We explain the safety and what to watch for after the procedure.
Most reactions are short‑lived and can be managed at home. You may experience pelvic pain, nausea, or a mild illness. These symptoms usually go away in a few days.
Common short‑term issues
- Pelvic discomfort, mild fever, and urinary urgency or burning that usually resolve in days.
- Bruising or a small hematoma at the catheter’s entry point are access-site effects.
- We recommend rest, hydration, and over‑the‑counter pain control unless we advise differently.
Less common and rare events
Some people might see blood in their urine, semen, or stool. You could also get a bladder spasm or a urinary tract infection. These might need antibiotics.
| Issue | Typical timing | Usual care |
|---|---|---|
| Post‑procedure pain/fever | First 1–5 days | Rest, acetaminophen, fluids |
| Access‑site bruising/hematoma | Immediate to 2 weeks | Pressure bandage, avoid heavy lifting |
| Blood in urine or semen | Days to weeks | Usually self‑limited; call if heavy |
| Rare non‑target effects | Immediate | Prompt evaluation, imaging checks |
“Call us for persistent fever, severe pain, inability to pass urine, or signs of infection at the access site.”
Recovery Timeline and Results You Can Expect
Recovery after this treatment is usually quick, with most patients leaving the hospital the same day.
Same‑day discharge, activity guidance, and medications
We keep a close eye on you for a short time to check the site and urine output. Most people go home the same day after a roughly two‑hour procedure.
Home care includes bandage care, staying hydrated, and light activity for 24–48 hours. Avoid heavy lifting or strenuous exercise for a week.
Medications: We often suggest over‑the‑counter pain medicine and a short course of antibiotics to lower infection risk. We also advise when to restart regular prescriptions.
When urinary symptoms typically improve
Many patients start to feel better within a few weeks. Noticeable improvement is often seen by one month.
Urinary symptoms continue to improve over the next several months as the prostate remodels. Expect ongoing gains up to about six months.
Durability of outcomes over time
Centers report long-lasting benefits for years. About 80%–90% of patients see significant symptom improvement and sustained relief.
We schedule follow‑up visits, symptom check‑ins, and tests as needed to track progress and treat any concerns such as infection or persistent urinary issues.
“Most people return to normal activities quickly and see steady symptom improvement over months.”
How PAE Compares to TURP and Other BPH Treatments
When looking at treatment options, we consider how well they work, how fast you recover, and how they affect your life in the long run.
Effectiveness: Prostatic artery embolization (PAE) is a well-established treatment for BPH. It offers lasting relief from symptoms and better urine flow. Studies show that many patients see improvements that last for months or even years.
Side effects and continence: PAE tends to have a lower risk of incontinence and fewer sexual side effects than surgeries like TURP. This is a big plus for maintaining quality of life.
Recovery and logistics: PAE is often done without general anesthesia and doesn’t require a hospital stay. This means a quicker return to your normal life compared to surgery.
- We compare symptom relief and flow — both approaches help, but treatment choice depends on anatomy and goals.
- We point out that compared to certain surgeries, PAE has lower rates of sexual and urinary side effects.
- We emphasize shorter recovery, less time in hospital, and fewer anesthesia risks for many patients.
Safety and choices: The best option depends on your anatomy, past treatments, and personal goals. If symptoms come back, there are other procedures or surgical options available.
“Our goal is to minimize risks while aligning the procedure with the patient’s priorities.”
Our Interventional Radiologists, Technology, and Patient‑Centered Care
Our team combines specialized skill with advanced imaging for precise, patient-focused care. We ensure clear communication and careful planning for each visit, making it efficient and reassuring.
Board‑certified expertise and advanced 3D X‑ray imaging
We introduce our board‑certified interventional radiologists who have focused experience performing this procedure safely and effectively. A dedicated radiologist leads pre-procedure planning and real-time navigation.
Our advanced 3D X-ray systems enhance visualization of prostate artery anatomy. Better views mean more accurate targeting and fewer surprises during the case.
FDA‑cleared embolic agents and safety protocols
We use FDA-cleared embolic agents chosen for this treatment and follow strict safety checklists to protect surrounding organs and limit non-target delivery of particles that affect blood flow.
- Pre-procedure planning sessions align technology, expertise, and patient goals.
- We provide clear education, attentive follow-up, and direct access to our care team.
- Continuous training, quality assurance, and research participation keep our care current.
“We focus on precise navigation, proven materials, and compassionate follow-up to improve outcomes.”
Conclusion
In summary, we find that catheter-guided treatment offers many patients effective relief with minimal downtime.
Prostatic artery embolization (pae) addresses the root cause of obstructive symptoms by reducing prostate size over time. Many men report symptom improvement within weeks and continued gains over months.
Advantages include outpatient care, local anesthesia, and a faster recovery compared with major surgery. Results can be durable for years in selected patients with BPH or prostatic hyperplasia.
We invite you to discuss goals and concerns with our team. The path forward is simple: consultation, focused evaluation, a tailored procedure plan, and dedicated follow-up to track outcomes over time.
FAQ
What is prostatic artery embolization and how does it help benign prostatic hyperplasia?
We use a minimally invasive technique called prostate artery embolization (PAE) to stop blood flow to the enlarged prostate gland. Using catheter-based techniques guided by imaging, our interventional radiologists place tiny particles into the prostate blood supply. This causes the gland to shrink over time and often relieves lower urinary tract symptoms such as weak stream, urgency, frequency, and nocturia.
Who is a good candidate for this treatment?
Men with moderate to severe urinary tract symptoms from benign prostatic hyperplasia who want a less invasive alternative to surgery often benefit. Candidates typically undergo symptom scoring, a clinical exam, and imaging. We consider prostate size, urinary retention history, prior urologic procedures, and overall health when recommending PAE.
How do we evaluate patients before the procedure?
We start by checking symptom scores and medical history. We also do urinalysis, digital rectal exam (DRE), and PSA testing if needed. Imaging like transrectal ultrasound or prostate MRI helps us understand gland size and blood flow.
This information helps us plan the procedure safely and effectively.
What happens during the procedure?
We make a small puncture in the wrist or groin to access the arteries. Then, we guide a catheter to the prostate under X-ray. We use an arteriogram to map the vessels and deliver embolic agents to block blood flow.
We treat both sides of the prostate when possible. We watch patients closely after the procedure for any pain or issues with urination.
What should patients expect right after PAE?
Most patients go home the same day. They get instructions on what activities to avoid and may need pain control and antibiotics. Some may feel pelvic pain, low-grade fever, or urinary irritation, known as post-PAE syndrome.
This usually goes away within days to weeks. Minor bruising or hematoma at the access site can happen but usually heals on its own.
How soon will urinary symptoms improve and how durable are results?
Many men see symptom improvement within weeks, with more gains over three to six months as the prostate shrinks. Results are usually long-lasting for most patients, but can vary. We check on symptom scores and imaging as needed to see how well the treatment works over time.
What is the difference between transurethral resection of the prostate (TURP) and PAE?
PAE has a lower risk of urinary incontinence and sexual side effects. It avoids general anesthesia and hospital stays. TURP may provide faster relief but has higher complication rates. We discuss the benefits and risks of each option with patients.
What are the main risks and side effects we should know about?
Common side effects include pelvic pain, urinary urgency, and low-grade fever. At the access site, there is a possibility of infection, bleeding, or bruising. Less common risks include blood in urine or stool, bladder spasm, and urinary tract infection.
Major complications are rare when done by experienced radiologists using modern technology and safety protocols.
What technology and safety measures do we use?
We use advanced 3D X-ray imaging and selective arteriography to map prostate vasculature accurately. We follow strict infection-control protocols and use FDA-cleared embolic agents. Our team of board-certified radiologists with experience in vascular access and prostate interventions ensures safety and effectiveness.
How should patients prepare and what is recovery like?
Preparation may include stopping certain medications, fasting, and arranging a ride home. Recovery is quick, with same-day discharge and limited lifting for a few days. We provide detailed instructions, prescriptions for pain control, and follow-up appointments to monitor progress and manage any complications.


Post Comment